The uneven impact of COVID-19 on communities of color and other marginalized populations in the United States threw the issue of healthcare disparities into sharp relief when the pandemic began. The amplified evidence of long-standing imbalances in social determinants of health and access to care raised the country’s collective consciousness.
As that happened, healthcare executives’ perceptions began to be transformed as well.
That’s a good thing, because healthcare organizations face the ongoing work of ensuring access to care for their most vulnerable patients as they continue to grapple with ongoing pandemic-related hurdles. They need all the insight into disparities they can get.
A Wake-Up Call for Providers
And they’re learning. More healthcare organizations have begun collecting data to pinpoint the gaps in their communities, observes Kedar S. Mate, MD, CEO, Institute for Healthcare Improvement.
For many, the insights gleaned from the analytics have offered a wake-up call. “People don’t like to see that they’re treating populations inequitably. No one likes to have that happen on their watch,” Mate says
The disparities so vividly displayed during the pandemic catalyzed an epiphany of sorts among healthcare leaders.
Pre-COVID-19, IHI surveys showed health equity to be near the middle or bottom of healthcare executives’ spectrum of priorities, according to Mate. Responses to disparities initiatives were favorable but not overwhelming.
The crisis crystalized their focus. The percentage of healthcare leaders who named disparities as one of their organization’s top three priorities more than doubled from 25% to 58% between 2019 and 2021. Disparities ranked nearly as high as safety, which 59% of respondents named a top three priority. “Health equity was the biggest delta in that two-year window,” Mate says. “The pandemic and the racial justice movement generated a crucible for the will to work on this issue.”
The American Hospital Association reports similar findings. Although the AHA Institute for Diversity and Health Equity’s last biennial survey, completed in 2019, revealed a strong desire among health systems to tackle equity, the data suggested organizations were doing more planning than executing, says Priya Bathija, the AHA’s vice president of strategic initiatives.
Enter the new coronavirus, which thrust inequities into the spotlight. Though data from the 2021 survey won’t be available till the end of 2022, “in speaking with leaders about how their work has changed over the past two years, we’re seeing hospitals start to close that gap between planning and doing,” Bathija reports.
Denver Health: An Equity Innovator
For Denver Health, there never has been a gap between planning and doing. As one of the state’s largest providers of Medicaid services, Denver Health exists to serve vulnerable patients, 90% of whom live at 200% or less of the poverty level.
The organization runs a 555-bed flagship hospital as well as 10 federally qualified community health centers and 19 school-based clinics in the city’s poorest neighborhoods.
Denver Health has used its experience in dealing with social risk factors to serve as a powerful safety net during the pandemic, and as an incubator for innovation.
“It’s hard for people to connect to large institutions, so meeting them where they are, in the settings that are important to them, is a critical part of our strategy,” says CEO Robin Wittenstein, EdD, FACHE.
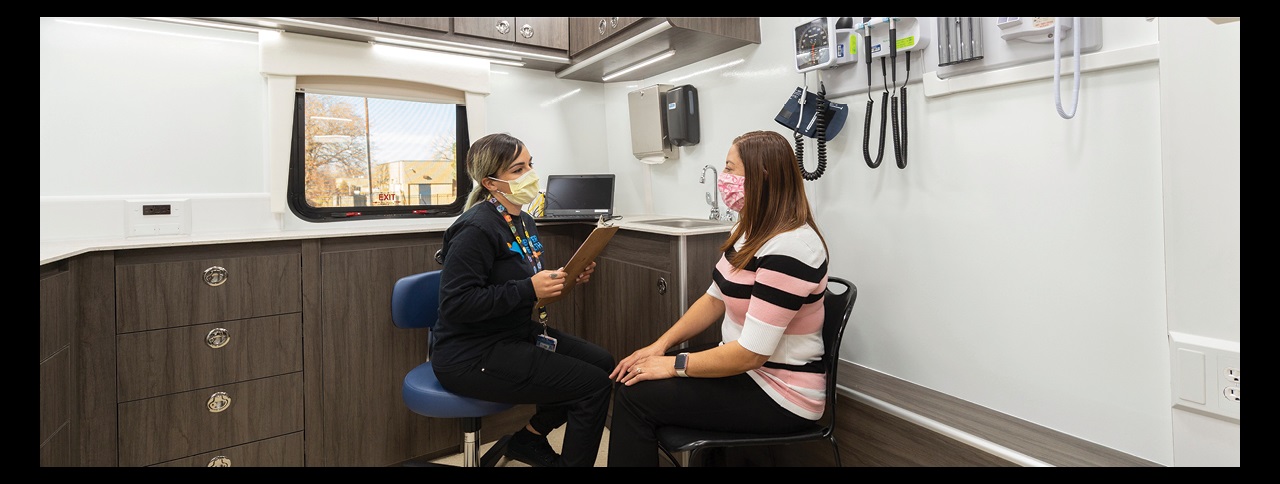
As COVID-19 surged in the community, it became even more critical for Denver Health to increase access to people in some of the hardest hit neighborhoods, many who didn’t have a primary medical home. In response, it deployed mobile health vans for COVID-19 testing and vaccines.
The program leverages connections with churches, mosques, libraries, recreation centers and homeless shelters to reach patients. Public health workers also connect with homeless individuals on the street.
“These efforts are a powerful way of demonstrating to patients that, in a moment of crisis, healthcare sees their challenges and is willing to come to them,” she says.
Denver Health kept its well-child clinics open so newborns and toddlers could continue to receive immunizations and care. “Keeping our finger on that pulse is critical, even in the face of COVID,” she says.
Other projects include:
- A hypertension management pilot project with the Denver Housing Authority that provides virtual healthcare via a telemedicine suite in a subsidized residence for patients who do not have access to electronic devices. Patients receive a Bluetooth-enabled blood pressure cuff and blood pressure education.
- An initiative to address lower immunization rates among Black children stemming in part from distrust of vaccines within the Black community. Denver Health is using its large dental care program as a vaccination site and conduit for discussions with parents.
“We need to understand where we touch patients and build opportunities to close the gaps into every one of those encounters,” Wittenstein says.
As the hospital was stretched to capacity caring for the sickest COVID-19 patients, it also created a nationally recognized virtual hospital-at-home program for low acuity patients.
Patients were given a package of tools to care for themselves at home and received regular calls from physicians and nurses. If their health began to decline, patients were immediately brought by ambulance to the hospital. The program has served 1,300 patients.
“Care can be retooled to meet the changing needs of patients in the most appropriate setting,” Wittenstein says. “Keeping patients out of the hospital should be the goal of every health system in the country.”
Memorial Community Hospital and Health System: Leveraging The Small-Town Advantage
With a minority group population of 5.3% and a poverty rate of less than 10%, Memorial Community Hospital and Health System’s demographics differ from those of Denver Health, but the two organizations share a common belief in the power of community partnerships.
When the COVID-19 vaccine became available and the Blair, Neb.-based provider realized that none of its clinics would be large enough to handle the volume of patients getting it, an employee suggested reaching out to an athletic training facility occupying the campus of a local community college that had closed 10 years earlier.
The facility had an unused gym with the perfect layout, including a large hallway. MCHHS used the site to deliver more than 900 vaccines daily.
“This is the value of community partnerships,” says Manuela Banner, RN, FACHE, president and CEO. “This facility had nothing to do with healthcare, but vaccinating our patients would’ve taken a lot longer without this access.”
Initially, MCHHS used its EHR to stratify high-risk patients and cared for many of them through virtual visits or by phone. “Once we learned more about COVID safety, we encouraged them to come in because we didn’t want them to miss their preventive care,” she says.
To maintain access to care during COVID-19 without jeopardizing safety, MCHHS saw healthy patients in the morning and sick patients in the afternoon to keep the two populations separate.
Still classified as a rural provider despite its location only 20 minutes from Omaha, MCHHS serves a community of 27,000 patients spanning two counties. The relatively young, affluent population makes the service area something of an anomaly among rural providers.
MCHHS’s most recent community health needs assessment revealed behavioral health and substance abuse as the top unmet needs, with lack of transportation for these patients following close behind. Within the school population, bullying (electronic and physical), alcohol use and vaping emerged as significant concerns.
To address these issues, MCHHS is developing an integrated mental health service at its primary care clinic. The goal is to increase access to behavioral healthcare for youth and adults by locating a behavioral health professional in the same place where patients see their family doctor.
“An integrated service removes some of the stigma of going to a counselor,” explains Banner. The model also gives family practitioners real-time access to a behavioral health professional if they identify a patient in need.
While the integrated mental health service is still in the planning stages, an outpatient on-site group therapy program led by a nurse case manager specifically for older adults dealing with loss, depression and other mental health issues has gotten off the ground. Psychiatric care via telehealth is available as needed.
Most participants come to the program via a robust referral process, and community outreach plays a vital role, with connections made through the Rotary Club, church groups and lunch-and-learn events at the hospital.
“Our key strategy is talking to all the community groups we can,” Banner says. “When it comes to medical care, being in a rural area has its advantages. A lot of times our connections and patients are our neighbors and family members.”
Mercy Medicine Free Clinic: A Medical Home for the Indigent
Like Denver Health, Mercy Medicine Free Clinic, Florence, S.C., exists to ensure access to care for the most vulnerable. One of 39 members of the South Carolina Free Clinics Association, the organization was chartered in 1994 to provide a free medical and dental home for the indigent, low-income and prison-release populations ages 18–64 in Florence, Williamsburg and Marion counties.
At any given time, 20% of the population qualifies as homeless.
Unlike Denver Health, Mercy Medicine Free Clinic is privately funded and does not accept federal third-party payers.
“Our niche is patients with virtually no income or those who fall below 200% of the poverty threshold,” says Wayne Jackson, FACHE, executive director. In addition to providing medical and dental care, the clinic takes referrals of patients lacking a medical home who seek nonemergent care in the ERs of Florence’s two medical centers.
“The case managers in those ERs have become good at identifying patients who meet our criteria. Treating these individuals with our private funding reduces bad debt for these organizations,” Jackson says.
Core providers consist of an internal medicine physician medical director, three nurse practitioners and a team of volunteer clinicians, including two nephrologists, four dentists, a pain management specialist, a physical therapist and a dietician. In addition to primary care, the clinic offers mobile mammographies twice yearly and mobile behavioral healthcare through the South Carolina Department of Mental Health’s Highway to Hope Project.
In 2021, Mercy Medicine provided more than 1,100 office medical visits and saw 250 unduplicated patients—a drop of about 50% from before the pandemic. Apprehension among unvaccinated patients and cutbacks in the city bus service had a chilling effect, Jackson notes.
When the vaccine became available, Mercy Medicine served as a vaccination center in cooperation with the Medical University of South Carolina. To tackle some people’s distrust of the vaccine, the clinic employed a strategy of culturally appropriate education and encouragement. “Our medical numbers are edging up,” Jackson reports.
Though patients must meet income criteria to receive care at the clinic, the massive job losses that occurred during the pandemic presented a unique circumstance. In response, the clinic created a program that relaxed the income requirements for participation, serving as a one-year stopgap for people who unexpectedly lost their jobs.
The clinic has also worked with the University of South Carolina School of Public Health on the development of a methodology to teach indigent patients how to ask questions of providers during appointments to maximize the benefits they receive from the visit and help improve outcomes. Plans are underway to introduce the methodology for implementation statewide.
A Lasting Strategy
The organizations profiled here are committed to opening more doors to care during the pandemic and beyond. And IHI’s Mate believes their care access strategy can change the way healthcare is delivered and vulnerable populations are treated in the U.S.
Mate points to signs that the commitment to advancing health equity and increasing access to care could last. One is the fact that public support runs deep. The new awareness of healthcare disparities has reverberated through all facets of society.
“For the next few years, we’re going to be talking a lot about equity, and some of that will stick,” Mate says.
To make sure it does, Mate and other public health leaders have called for the creation of a Quintuple Aim that adds advancing health equity to healthcare’s Quadruple Aim of better population health outcomes, better patient experiences, lower costs and workforce well-being.
This goal is needed because most of healthcare’s challenges in achieving the Quadruple Aim stem from lack of attention to the equity dimensions of healthcare, Mate and his colleagues argue in a JAMA Viewpoint article published Jan. 21, 2022.
Since providers’ ability to move toward value-based care depends largely on success around the four aims, integrating equity into all aspects of that work makes sense in terms of caring for patients and of economic survival, Mate says. Advancing equity is good for people and good for the business of healthcare, too.
“There’s no single playbook for advancing health equity,” Bathija says. “It’s important for leaders to focus first on understanding what’s happening in their communities. We’ll never be done, but we can continue to understand, test, improve and mature.”
Susan Birk is a Chicago-based freelance writer specializing in healthcare.